The Ear – Is it the Problem, Or Not?
Ears are often blamed as the cause of many problems. These include pain, plugged head sensation, dizziness, muffled hearing, and unwelcome sounds such as crackling and humming. Although ears can be among the peskiest sources of discomfort for both children and adults, people are often surprised to find they are not always at the root of these problems.
A basic review of ear form, function, and facts will help explain why the ear often gets such a bad rap. For better clarity, let’s break the ear down into two separate areas: The outer ear and the middle ear.
(Note: We aren’t forgetting about the inner ear, which includes structures involved with balance and interpreting sound. But the inner ear is pretty complicated and doesn’t “feel” pain, so to speak. So we’ll enjoy a discussion about those inner structures at another time and focus first on the more accessible parts.)
The outer ear
The form
The part of the ear that you see on the sides of your head consists of skin-covered cartilage. There are lots of anatomy terms you could learn if you’re into it–concha, pinna, tragus, auricle, helix, and several more. All those areas that jut out, fold or curve are called by standard names, as any experienced piercer will tell you.
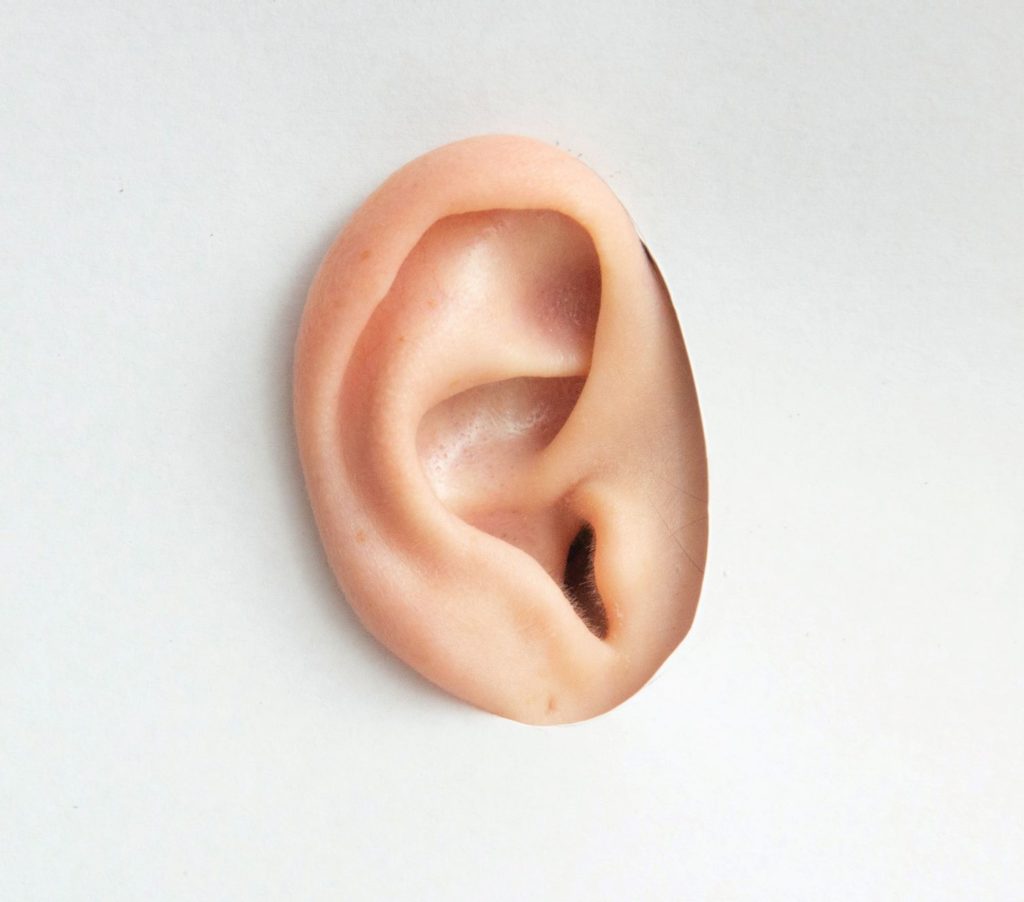
The part of the outer ear that isn’t so obvious is the canal that tunnels inward. (Yes, in medical terms, the inward-leading canal is still called the outer ear.) It is constructed from skin-covered cartilage and bone. Although the canal is only about an inch long, it usually has a small bend with an even narrower section toward the middle. Over the skin is a fine hair network and, ideally, a thin layer of sticky wax.
The function
Love or hate how they look, the outer ear’s basic purpose is as a sound collection dish and conduit to the sound transfer center (see section below on the middle ear). Owing to the canal’s bend, hairs, and coating of wax, it is fairly effective at protecting the sensitive structures within from unwelcome matter like dust or insects.
Interesting facts
- Earwax originates just inside the canal as a liquid substance similar to oily sweat. This can explain why your canals at times feel mildly wet without obvious cause.
- The external canal in adults is only about 1/4 inch wide. Which is why trying to clean the canals with a cotton swab just pushes the wax farther in.

- Wax is acidic, and therefore good at hindering germ growth to prevent infections.
- Some peoples’ canals make wax that is much drier than others–it’s largely determined by genetics. Earwax moves slowly out of the canal on its own, aided by jaw movements. In general, wax that is too dry or thick is more difficult to move. So, if your ear wax is dry or built up, you can consider placing a drop or two of unscented mineral oil in your canals each month to assist in their clearance of wax.

Problems
- Other than earwax blockage, one of the most common problems of the external ear is bacterial or fungal infection of its skin surface. This is much more likely to happen in wet environments (such as frequent swimming) or when the protective mechanisms discussed earlier are disrupted. It can occur even from microscopic scrapes caused by enthusiastic (and ill-advised) cotton swab use. Ear structure pain when you lay or pull on it can be a sign of a canal (external) infection.
- If your outer ears are very itchy or flaky over a period of time, you may have eczema or psoriasis. This can be true even if you don’t have it on other parts of your body.
- Because the ears tend to jut out from your head, they are at high risk for sun damage. Be sure to cover them well with sunscreen and report skin changes to your health care provider.
The middle ear
The form
The business side of the middle ear is made from the eardrum (tympanic membrane) and the tiny bones of hearing (ossicles) attached in series on the other side. Many of us think of these bones by their common names, the “hammer,” the “anvil,” and the “stirrup.” Most of the rest of the middle ear consists of a very small vault of empty space of normal air around the little bones.
In some ways, the tympanic membrane well fits its common term, “drum,” with a structure similar to the clear drumhead in the picture below. A healthy eardrum is so transparent you can see through it to the tiny bones on the other side. Like the drumhead, it is sealed tightly around the edges and won’t let substances like water or air pass from the outer ear to the middle ear vault. In adults, the eardrum is only about as wide as a typical pencil eraser.

The structure of the eardrum, however, is a bit more complicated than it seems. Though it can be virtually see-through, it consists of three different layers of living tissue. The layer that faces the canal is skin-like and covers a more fibrous middle layer. The inner layer, facing the ossicles, is a mucus membrane similar to the lining of the inside of your nose.
The function
The middle ear’s primary function is to amplify and begin to interpret sound. As sound waves reach the middle ear, how they amplify and transmit to the tiny bones from the eardrum is a remarkable process. If you want to learn more about it, click here for a simple explanation. For those interested in the biophysics of sound interpretation, you can look at an article like this one.

Interesting facts
- The eardrum has good blood flow, especially in children. Often when a provider looks at a crying child’s eardrums, they are red, much like the child’s face. The same tends to be true if a fever is present, when the face is red and flushed.
- Like the inside of your nose, the inner layer of the eardrum can produce mucus when it is inflamed. When it is irritated it will likely feel uncomfortable or itchy. This can be a normal part of an illness, depending on several factors. Mucus and even bacterial overgrowth in the middle ear often go away on their own.
- When there is mucus or fluid behind the eardrum, it’s very difficult to test it by lab culture to see if it is caused by bacteria. This means that a provider has to make an educated guess about whether to treat an infected-looking ear with an antibiotic.
Problems
- As mentioned above, when your eardrums are inflamed because of a cold, allergies, or other irritation, mucus or fluid can accumulate on the inside of the eardrum. When the process gets carried away, there can be pain, muffled hearing, feeling off-balance, generalized illness or even a broken (perforated) eardrum if the pressure is too high. A perforation can actually relieve pressure and may help prevent deeper infections. The tear in the eardrum often heals on its own without causing permanent damage.
- The ear canal and eardrum sense pain using the same nerves (five or six of them!) as do parts of your teeth, jaw, face, neck, and more. Because of this, it can be difficult for your brain to correctly interpret the true source of the pain. In other words, pain that seems like it is coming from your ears may have nothing to do with your ears at all.

Putting it all together
In my practice in clinic, most adults with ear pain tell me an “ear infection” is the reason for their visit. Yet, about half of those patients have very normal-looking canals and eardrums. I estimate that only 1 or 2 out of every 20 adults I see with ear pain meet evidence-based criteria for antibiotic prescription.
It’s good to know this because it can help you expect that a visit to your health care provider for ear pain may reveal no ear abnormalities at all. Or may result in a visit in which you do not receive a prescription for relief.
A really good idea if your provider offers you an antibiotic for ear pain, or any other treatment, is to ask the risks and benefits of using or declining the treatment. “How sure are you that I really need this medicine (or treatment, etc.)?” and “Is the expected benefit worth the risks?” can be good ways to ask questions.
If the ear isn’t the problem, what is?
A really thorough investigation into other issues–inflammation of nearby structures, tooth or TMJ (jaw) abnormalities, even obstructive sleep apnea–is usually warranted when there are ongoing problems for which there seem to be no other explanation. Ear, nose and throat (ENT) specialists are great resources for looking into issues that drag on.

The real culprit responsible for many of the problems we mentioned at the beginning of this article–ear “popping,” feeling of fullness, pain, and so forth–is often dysfunction of a body part that it is impossible to see in a regular clinic: the eustachian tube. It isn’t technically part of the ear, but it certainly can have a direct impact on ear comfort and function. Look for a more thorough discussion of the eustachian tube in future topics.
Meanwhile, the next time your ears hurt or seem to cause trouble, cut them some slack and consider that the source of the problem may not be your ears at all. And do your best to take good care of them!
Health topics on IllumiMed are intended to convey information that can help improve health literacy. The provider opinions and explanations expressed by Carissa Arens, APRN, CNP derive from years of scholarly investigation, work in clinical settings and as a formal health care educator. The topics do not replace competent medical care. For more information, see our post describing the main purpose of our site.
Sign up for all of the well-researched medical knowledge we can convey as fast as we can type (and that's pretty fast!).
Don't miss a single thing.
JOin our list
Are you in need of non-emergency,
no-cost health services?
YES
(Opens new window to schedule)
NO
(Closes this popup)
(Minnesota residents only)
ADD A COMMENT
December 17, 2020